The article about Pediatric Associates in CA has a nugget with a potentially outsized impact: the implication that VFC vaccines…
News 3/30/10
From Friend of Don: “Berwick as CMS chief. WOW, WOW, WOW!!! You know he’ll want to change reimbursement schema from volume to value based on day one. Wonder if he’ll be able to turn that big ship in his lifetime?” Dr. Donald M. Berwick runs the Institute for Healthcare Improvement and is a pediatrics and health policy advisor at Harvard. He’s a big advocate of providing better care at a lower cost believes the government and insurers can increase healthcare quality of efficiency by basing payments on the value of service rather than volume. I also noticed a more obscure fact about Berwick: in 2005, he was bestowed an honorary Knight Commander of the Most Excellent Order of the British Empire for his help reforming the NHS.
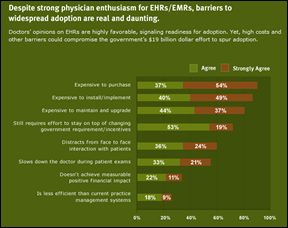
Sermo and athenahealth release results from a Physician Sentiment Index that indicates doctors aren’t too happy with the business of medicine. A couple of the more disturbing findings: 59% of physicians think the quality of medicine will decline in the next five years and 64% agree their clinical decisions are being based more on what payors are willing to cover than what they think is best for their patients. Not surprisingly, physicians still think EHRs are too expensive to buy, implement, and maintain. Sermo CEO Dr. Daniel Palestrant explains the results in more detail in this CNBC interview.
eClinicalworks says it has implemented 2,000 providers across 400 independent practices in New York City over the last two and half years. Another 600 providers and 100 practices are in the implementation process.
And in the Midwest, physician network Advocate Physician Partners partners with eClinicalWorks and will recommend eCW’s PM/EMR to its 2,600 independent physicians.
North Florida Surgeons selects Allscripts EHR/PM solution for its 34-provider practice. The practice’s CEO says that a key reason they selected Allscripts was the availability of Allscripts Patient Payment Assurance module to to calculate patient responsible amounts and secure payment authorization prior to surgery.
MinuteClinic names Nancy J. Gagliano, MD as chief medical officer. She most recently served as SVP of practice improvement for Massachusetts General Hospital and Massachusetts Physicians Organization.
Theft of personal health information grew from 3% in 2008 to 7% in 2009. Over 275,000 case of medical information theft was reported in the US last year. With increased EHR adoption, medical identity theft is predicted to increase. Furthermore, criminals use information from medical records for 320 days versus 81 days with other types of identity theft. Medical identity theft also takes twice as long to detect.
In more optimistic EHR news, a new NEJM paper supports the use of EHRs to help physicians make more accurate diagnoses. The physician authors believe EHRs can help diminish diagnostic errors in numerous ways, including:
- filtering, organizing, and providing access to data
- fostering thoughtful assessment and collaboration between physicians and patients
- facilitating the documentation of patients’ ongoing and evolving history
- providing better tools for managing patient problems
- ensuring fail-safe communication and action in ordering tests and tracking the results
- incorporating checklist prompts to ensure key questions are asked and relevant diagnoses considered
- providing automated follow-up systems and patient educational tools.
The authors admit that the current generation of EHRs don’t necessarily provide these benefits, but they envision a “redesigned documentation function” that includes improved tools for making diagnoses.
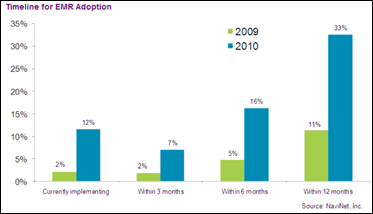
EMR adoption appears to be trending up for practices with 10 or fewer physicians, with 33% of offices planning to implement an EMR within 12 months compared to 11% in August 2009. I was surprised to see that only a quarter of the groups will seek ARRA incentives and a whopping 63% were unaware or unsure of the meaningful use reporting requirements. I’m assuming that latter group doesn’t follow HIStalk too often.