The article about Pediatric Associates in CA has a nugget with a potentially outsized impact: the implication that VFC vaccines…
Pretzel Logic: Technology Decision-Making for Medical Practices 3/30/11
Meaningful Use, Chapters Two and Three
So now that you’ve got Meaningful Use Stage 1 out of the way, it’s time to start focusing on Stages 2 and 3.
OK, I’m kidding. But still, before you jump on the MU “escalator” (as the good folks at ONC like to call it), it may be worth taking a tiny peek at what Stages 2 and 3 might have in store. Not only for the morbid fascination of it, but also because it gives you some hints and clues about what might be waiting for you at the top of the “escalator.”
Where might we look for such clues? Why, the Meaningful Use Working Group (MUWG) of the Health Information Technology Policy Committee (HITPC), of course. This is a federal advisory group that provides advice to ONC on — you guessed it — Meaningful Use.
While the MUWG only makes recommendations and has no ability to create law or regulation, if history is any guide, their recommendations are likely to be the foundation for what eventually becomes regulation. [Full disclosure: I am not formally a member of the MUWG, but as a member of other WGs I do occasionally participate in their deliberations.]
On January 13, 2011, the first recommendations on Stage 2 and 3 were put out on the ONC website for public comment. The comment period is now closed. On April 5, the WG will have a public hearing to discuss the public comments that were received. You can see those recommendations here.
Just what was in those recommendations? You may recall that MU Stage 1 has 25 possible requirements for Eligible Professionals (i.e., ambulatory clinicians), of which you have to meet 20. Start with the 15 “core” set items that are required, and then choose five from among 10 in the “menu” set.
Note: I should point out that I’m going to focus only on physician requirements, not hospital. I’m less familiar with hospital requirements and, unlike hospitals, most physician offices don’t have staff who keep track of all of this mumbo jumbo.
For each requirement, there is an objective, which is what you have to do (“record demographics”), and a measure, which is how much of it you have to do (“for 50% of patients.”) The MUWG started with these 25 Stage 1 requirements and then built from there to get to Stages 2 and 3.
In some cases, they recommended that a Stage 1 requirement just continue into Stage 2, meaning that you just need to keep doing what you’re doing in order to keep getting your incentive payments. Some Stage 1 requirements that were optional “menu” items become “core” in Stage 2. In other cases, they raised the bar on an existing requirement by either increasing the measure (“go from 50% to 80%”) or increasing the scope (“go from CPOE for just medications to include radiology and labs”). And, of course, they also had some genuinely new recommendations.
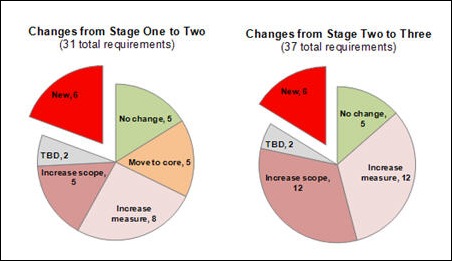
A summary breakout of their recommendations is above, showing how requirements move from Stage 1 to Stage 2, and then from Stage 2 to Stage 3.
Going from Stage 1 to Stage 2, relatively few measures are left completely unchanged. Everything else is either made mandatory (which is unchanged if you chose any of those in Stage 1) or increased in some substantial way. And, there are six totally new requirements.
Going from Stage 2 to Stage 3, five measures are untouched from Stage 2, while a whopping 24 are increased in some way and six new ones are added to boot.
Bottom line is that, as promised by CMS and ONC, the requirements are increasing over time. Some are increasing in ways that are easy to predict, while others, like new measures, are much harder to anticipate.
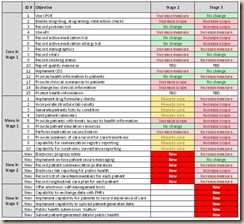
Of course, the devil is in the details. The table above (click to enlarge) shows how each of the requirements fares over the movement from Stage 1 through the middle passage of Stage 2 to the distant horizon of Stage 3.
The full descriptions (such as they exist) are on the ONC website per the link provided earlier. You can get a good description of the original Stage 1 requirements here.
So, what you should take away from all of this? Remember, these are just recommendations from an advisory group, so there’s a lot of process between here and the actual requirements that you’ll be responsible for. That said, they are strong leading indicators and do suggest some general guidance.
First, this isn’t an “escalator” or a “fast-moving train” or any other non-weight-bearing analogy. This is a climb, pure and simple. Your committing to this climb is, unfortunately, without the benefit of knowing what mountains, cliffs, whitewater, and mountain lions lay over the first hill.
Second, you can run but you can’t hide. Almost all of what is optional in Stage 1 becomes mandatory in Stages 2 and beyond. Choose what’s easiest and manageable in Stage 1, but don’t be blind to what’s just over the hill.
Finally, beware of the “TBDs,” especially the quality measures. Many have found that the quality measures are their own set of MU requirements. There is a separate Quality Measures Working Group that is hard at work looking at new measures. There is no doubt that we can’t improve what we can’t measure, but it is all too easy for those who are not familiar with EHRs to assume that they yield quality measures easily and accurately. They do not.
One concern that I have with all of this is with the timelines. The first cohort of MU over-achievers can start attesting to Medicare on April 18. They’re going to be required to start on Stage 2 on January 1, 2013. That’s not as far as away as it sounds if you think about the bureaucratic steps that need to be taken and the lead time needed for vendors to develop their products, get them certified, and train clinicians to use them.
I’m also concerned that many of the new requirements are trying to use MU as a lever to accomplish other objectives, such as public health goals and patient engagement aims.
The biggest concern for physicians is that many aspects of these new requirements are out of their control. Hopefully the public feedback to ONC that we’ll hear about on April 5 will quell the attempt by policy-makers to use physicians as the hammer to attack every nail, staple, rivet, and railroad spike.
Micky Tripathi is president and CEO of the Massachusetts eHealth Collaborative. The views expressed are his own.


Great piece.
My only quibble:
“I’m also concerned that many of the new requirements are trying to use MU as a lever to accomplish other objectives, such as public health goals and patient engagement aims. ”
Um, haven’t those been among the obvious goals all along? If not, why even bother?
Again, though, great piece.
Nice article, Micky. You stated “The first cohort of MU over-achievers can start attesting to Medicare on April 18. They’re going to be required to start on Stage 2 on January 1, 2013. That’s not as far as away as it sounds if you think about the bureaucratic steps that need to be taken and the lead time needed for vendors to develop their products, get them certified, and train clinicians to use them.”
This makes me wonder: Is there any vendor input to MUWG? If so, what and who?
Nice piece, brought to mind what an old plumber told me one time. He said,”Greg just remember that they can kill you but they can’t eat your clothes”.
Thanks everyone for your kind words.
To RustBeltFan: The MUWG has one vendor on it — Seimens. They report to the HIT Policy Committee which Epic is a member of. Every one of their meetings is open to the public and has opportunity for public comment so anyone — vendor or otherwise — can provide input to the WG. For details on the membership of the workgroup and all of their meeting materials go to the ONC website and follow the link to Federal Advisory Committees.