The article about Pediatric Associates in CA has a nugget with a potentially outsized impact: the implication that VFC vaccines…
News 4/3/12
From Santiago: “Re: EMR and merging practices. I read more details about the former Northwestern Memorial Physician who resigned and blames the practice’s computer system for inefficiencies. Apparently he had been in solo practice for 12 years and used a different EMR before joining Northwestern. I think people need to realize that we will have more issues with physicians who are forced to change EMRs when practices merge. If one is used to a certain EMR, it’s not an easy task to change, nor is it inexpensive. And, the older the doc, the harder it is to get them to change.” Santiago is referring to the Chicago physician who is now in the midst of a law suit with his former practice. He’s right: more mergers and acquisitions means physicians will face the challenge of switching EMRs.
The AMA’s online newsletter points out some of the missed opportunities for practices that have not created an online presence. One consultant notes that even practices that don’t need to attract new patients should develop a Web presence since information about physicians and practices is already out there, just not under the control of the practice.
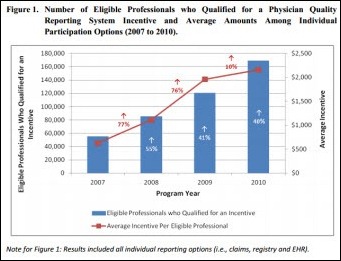
CMS paid $391.6 million in PQRS incentives for 2010, a 65% increase over 2009. A total of 268,968 healthcare professionals participated in the program and were paid an average of $2,157 per individual and $20,364 per practice. Payments for the e-prescribing program jumped 83%, with CMS distributing $270.9 million to 65,857 individuals and 18,713 practices.
The administrator of a six-physician primary care group details her practice’s management of paper records in preparation for the group’s EHR go-live. After weighing several options, the practice opted to scan patients’ charts as they came in for appointments starting two months before the go-live. Eventually the practice was able to convert space once used for medical records storage into three exam rooms.
The AMA, MGMA, AAFP, and multiple other professional organizations send CMS a letter expressing their “profound concern about the imminent storm” of overlapping regulations affecting physicians, including e-prescribing penalties, the MU program, and the transition to ICD-10:
We urge CMS to re-evaluate the penalty timelines associated with these programs and examine the administrative and financial burdens and intersection of these various federal regulatory programs. We also urge CMS to use its discretionary authority provided by Congress under these programs to develop solutions for synchronizing these programs to minimize burdens to physician practices, and propose these solutions in the physician fee schedule proposed rule for calendar year 2013.
The Washington Post looks at initiatives in place at Stanford and Georgetown Universities that strive to teach medical students to maintain human connections with patients while using technology. Stanford advises students to face their patient, excuse themselves to check the computer screen, and put away gadgets when not needed. Meanwhile, Georgetown hires actors to portray patients during simulated exams that involve students accessing EMRs and explaining test results to their actor-patients.
More news: HIStalk, HIStalk Mobile.








Seamless connection?
Those who want a seamless connection with the universe (constellations) get see-through umbrellas and draw on them. At night (when it’s not cloudy) the umbrella makes one impression by combining documented information and reality. Search “star constellation umbrella”
Odd that only black ones are sold, not clear ones you can see through and use seamlessly, makes me wonder if EHR vendors, universities, et al. are fixated with black umbrellas.
So yes, I’m suggesting healthcare providers put medical records on clear umbrellas. Then they can look at the patient while reading.
It’d all seem so futuristic if heads-up displays were a myth.