Re: Walmart Health: Just had a great dental visit this morning, which was preceded by helpful reminders from Epic, and…
News 1/17/13
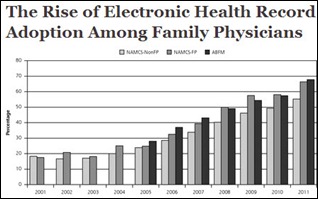
A study published in Annals of Family Medicine finds that EHR adoption by family physicians has doubled since 2005 and will exceed 80 percent by the end of 2013. Researchers also found family physician adoption rates were higher than those of other office-based physicians as a group, but say the reason is “unknown.” My theories: EHRs are better suited to the workflow of FPs; FPs are more motivated than higher-paid specialists to adopt EHRs and take advantage of MU incentives; and more low-cost EHR options exist for primary care physicians than specialists. Any other theories?
White Plume Technologies will offer its charge capture and coding solutions customers Wellcentive’s AccelaPQRS, a registry-based alternative to claims-based PQRS reporting.
GE Centricity resellers Alliance Healthcare Solutions and Final Support merge to form Quatris Health and become the largest VAR for GE Centricity practice solutions.
ACPE finds that only 12 percent of physicians find online physician ratings helpful. More than a quarter say the rating sites are a nuisance and over half don’t believe their patients have used one. However, 81 percent of the physicians who check their profiles think the ratings are at least partially accurate.
AMA submits comments to ONC urging that Meaningful Use Stages 1 and 2 be evaluated before committing to a Stage 3. It says its members most often express five concerns: (a) passing requires a 100 percent score; (b) the core measures are inflexible with regard to practice patterns and specialties; (c) the program needs to be independently evaluated; (d) EHR certification needs to place more emphasis on software usability; and (e) healthcare IT infrastructure barriers prevent data sharing. AMA wants three years between stages to give EHR vendors time to prepare – one year for making the rules, one for product development, and one for implementation.
The AAFP also submits comments that call for a delay of Stage 3 until at least 2017 and an elimination of all penalty provisions. It says HHS should (a) focus on problems that require coordination rather than wasting resources on criteria such as CPOE, demographics, lab results, and counting and verifying electronic prescriptions; (b) promote simplicity over complexity; and (c) require the implementation of measures that have broad, clinically-proven impact rather than experimental measures that may not be mature enough for the MU program.