The article about Pediatric Associates in CA has a nugget with a potentially outsized impact: the implication that VFC vaccines…
News 7/9/13
From Gloria: “Re: EMR features. Can you please help me understand if there is any major difference in EMR features for practices depending on the number of providers? For example, how would an EMR used by a solo physician differ from an EMR used by a large practice of 41+ physicians? Do both of them not do the same thing..namely treat the patient for conditions?” I am sure many readers can answer this better than me, but here are a few thoughts. While most EMRs include the same basics, such as the ability to track patient history and capture clinical notes, EMRs used by larger groups tend to include more features and functionality. For example, many EMRs catering to small primary care practices have less developed templates and rely more on free-text data entry. Larger groups have a greater need for care coordination, especially if patients are seen by multiple providers within the same practice, and will likely seek a variety of bi-directional interfaces to automate high volumes of orders and results. The architecture behind an EMR is also important since a program designed for small offices may not scale beyond a handful of users. Beyond features and functions, many EMR vendors don’t have adequate training and support resources to satisfy the demands of large groups. Readers, please offer additional insights.
The medical director for 70-provider South Texas Medical Clinics says its recent implementation of EMR has allowed the practice to “substantially” reduce its percentage of medical errors below the national average. I assume that STMC uses eClinicalWorks since it is part of Memorial Hermann Medical Group, a large eCW client.
The American Academy of Ophthalmology plans to implement an eye disease patient database that will enable ophthalmologists to statistically review and analyze their own care and compare it to benchmarks and peer physician performance. The Intelligent Research In Sight Registry (IRIS) will be populated with de-identified data collected from practices’ EHRs and serve as a PQRS EHR submission vendor.
HIMSS Analytics recognizes 31 Bon Secours Health Systems (VA) ambulatory clinics with the HIMSS Stage 7 EMR Ambulatory award for its implementation of Epic.
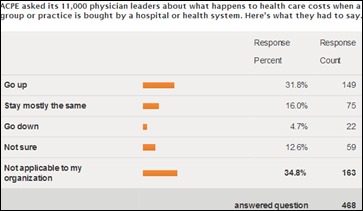
Almost one-third of physician executives participating in an ACPE survey believe that healthcare costs go up when hospitals buy physician practices.
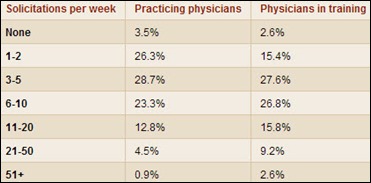
The doctor shortage and an improved economy has led to an increase in physician recruitment activities. A quarter of practicing physicians report receiving 24 to 40 job solicitations a month.




For Gloria: EMRs for large practices often have features related to different specialties or locations within a single practice. For example, staff can be assigned to a provider, providers can be grouped onto locations, there may be group as well as individual level preferences, and security is often more granular.
Large practices also often want more support for enforcing certain workflows and standards.
For Gloria: I’ll list a few additional aspects of potential feature/functionality differentiation between EMRs targeted to small versus larger practice settings. To generalize, it will be the degree of robustness of the functionality.
– Deeper scheduling functionality.
– More advanced billing and claims feature set, e.g. smaller EMRs did support UB-04 claims at one time.
– More comprehensive reporting package, such as functionality that can roll-up data across all groups or parse to specific data by provider, specialty, insurance type, diagnosis and gender. Might offer reporting modules (typically offered as add-ons) that support ACO analysis or audit reporting.
– The potential for Population Health modules (add-on) with features such as Patient Reminders, the ability to track and report on specific disorders for QM,PQRS or internal research projects, an Immunization tracking feature.
– More extensive support for the ability to interface/integrate with outside applications such as claims clearing houses, e-billing, e-fax, e-Rx, CCI-based coding applications, patient portals, speech recognition software, interface to QM and PQRS registries, interface to the state’s electronic Immunization Registry, imaging systems, documentation management systems. This potential for feature expansion, limited only by budget constraints, represents a key differentiator from my perspective.
Gloria, The EMR is a tool to support workflow. Think about the workflows that exist in the practice — and how they can be automated. It’s like listing the differences between a Volkswagon and a dump truck. They mean nothing without knowing what needs to be accomplished. Develop a full understanding of the practice’s requirements first. Until that’s done, there can be no context for deciding which EMR you need. All the features will look terrific but you may choose something that has no relevance to what is really needed.
Sorry for the late reply, busy at our Users’ Conference.
The 3 comments above to Gloria are generally spot-on. I take exception to many – but not all – of the items on non-sequitor’s list as being the domain of the large-practice vendors. At the very least, ARRA mandates a number of those features and all the small vendors I know (the market I live in) do many of these things, if not all. And often better than some of the big fish. But it’s an important point n-s made.
Two comments of my own:
– I notice that the line between EHR and PM is blurry above and in my conversations with doctors. Although the EHR/PM decision almost always goes hand-in-hand these days, I still consider anydiscussion about claims/clearinghouses/most reporting to be the domain of the PMS. For the purpose of your question, though, the responses above still ring true on the PMS side.
– I also note a disturbing trend of boiling down the quality of an EHR to its stated sum of features. This is a huge mistake, imo, and what leads to the high dissatisfaction rate docs have with their first EHR purchases. Your EHR is, imo, should be more about workflow, customer support, and where they will be in 5 years. Bells and whistles are almost meaningless.
And I’ll be the one to say this: the bigger vendors will, indeed, have more features/functions, but the smaller vendors will be more useable and practically functional. It’s no exaggeration to say that most of my clients (private practice pediatricians) would go out of business if they had to use any of the top 5 hospital vendors – just as we would be equally poorly suited in a hospital environment.