Re: Walmart Health: Just had a great dental visit this morning, which was preceded by helpful reminders from Epic, and…
News 8/29/13
From Sue Orman: “Re: Credit cards from payers. In addition to the exorbitant merchant fees, a problem with insurers using credit cards to reimburse providers is that there tends to be a lot of issues with practices not receiving electronic remits. That violates the spirit of administrative simplification under HIPAA and ACA. Not only does CMS need to make sure that payers are paying physicians their contracted rates, they need to encourage payers to immediately begin using the EFT standard ACH CCD+, which conforms with HIPAA and is less costly than credit card transactions.” Readers more familiar with the payer world and electronic standards can likely speak more knowledgably than me on this, but my understanding is that beginning January 1, 2014, payers will be required to accept EFT in the new standard format if requested by a provider. If a provider does not request the new format, the payer can continue using credit cards for reimbursements, which translates to more fees and less money in the hands of the physician.
eClinicalWorks names HealthNet (IN) the winner of its Improving Healthcare Together video contest. Auburn Medical Group (GA) and Open Door Family Medical Centers (NY) took second and third places.
Doximity, which is like LinkedIn for physicians, now boasts 200,000 licensed physician members, or about 30 percent of the doctors in the country. The platform allows physicians to share patient information in a HIPAA-compliant format and look up colleagues or relevant specialists. Sermo, another physician-only online community has a reported 125,000 users.
HBMA introduces Professional Billing Service Locator, a free platform to help practices locate medical billing companies that serve their region and their specialty.
Physician RCM provider MedData promotes Ann Barnes from president to CEO.
The benefits of a practice’s ACO participation reach beyond the patients covered by the ACO, according to a JAMA-published study. Researchers found that medical groups’ participation in commercial ACOs was associated with savings for Medicare beneficiaries as well, though the quality of care for Medicare patients did not consistently improve. The “spillover” effects may be the result of organizational changes in care delivery, such as incorporating computer reminders to reduce unnecessary and expensive tests.
New York doctors must now check an electronic prescription drug database before writing prescriptions for painkillers and other controlled substances, and, pharmacists must consult the database before filling the prescriptions; pharmacists must also report in real-time when a prescription is filled. The requirement, the first of its kind in the country, is part of the state’s I-STOP law, which also mandates electronic prescribing for all drugs by December, 2014.
In HIT fashion news, Vestagen Technical Textiles secures $8.25 million in financing. The company develops a variety of textile products and technologies, including scrubs that don’t absorb liquids and thus protect workers from potential contaminants. I guess the scrubs’ practicality and safety benefits are suppose to make up for the lack of spicy colors and patterns.
The San Diego newspaper highlights some of the more innovative ways area physicians are using smartphone apps and other technology to engage patients and monitor such things as weight, exercise, blood sugar, depression, and medication adherence. My favorite: Scripps offers pre-recorded videos of doctors so patients can become familiar with their physician prior to the first appointment.
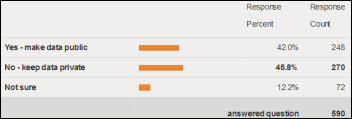
Physicians are split when it comes to whether or not Medicare should make data about Medicare payments available to the public, according to an ACPE poll. Forty-six percent of ACPE members participating in the survey are in favor of keeping the data private and believe the information could “too easily be misinterpreted by the public and be used to portray physicians in a negative and unfair light.” I am with the 42 percent who are in favor of transparency and believe the public has a right to know how tax dollars are being spent.
Email Inga.





The requirement to check a web site before prescribing controlled substances has been law in Ohio for at least two years (http://www.med.ohio.gov/pdf/rules/4731-11-11%20FAQs.pdf). It’s also the rule in Tennessee, Indiana, and Kentucky (the states where our providers do business) and likely true in most other states.
To say that the NYS PMP requirement is “the first of its kind in the country” seems to be inaccurate, unless I am misinterpreting the statement.
[From Inga] – NY lawmakers claim their program is the country’s first “real-time” prescription drug database because it is updated and available to providers as soon as the prescription is filled.