Re: Walmart Health: Just had a great dental visit this morning, which was preceded by helpful reminders from Epic, and…
News 4/29/14
Medfusion announces that its relationship with Allscripts has ended “due to unresolved payment disputes.” The termination is hardly a surprise given Allscripts acquisition of the competing JarDogs patient engagement platform last year. Medfusion says it will continue to provide uninterrupted services to the 30,000 Allscripts providers using its products through May 31, 2014; after that time customers wishing to remain on the Medfusion platform must contract directly with Medfusion.
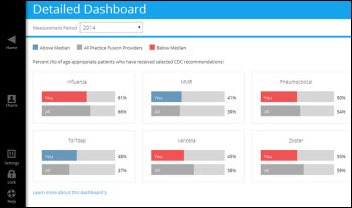
Practice Fusion launches a population health management offering in collaboration with Merck, giving practices a real-time dashboard that compares a provider’s patient vaccination rate with other Practice Fusion providers.
The HIMSS Electronic Health Record Association (EHRA) tells the ONC it opposes the proposed 2015 voluntary certification EHR criteria, saying that by the time the final rules are published there won’t be enough time for vendors to properly code and test enhancements. EHRA also argues that “more frequent certification is not desirable and would be costly.”

AAFP board member Daniel Spogen, MD rants about the administrative hassles of EMR in an AAFP blog post. Among his complaints: EMRs lack interoperability, are not user-friendly, take time away from patient encounters, result in mixed patient outcomes, increase overall costs, and complicate office workflow. I guess his only goal was to fire up his peers since he fails to suggest any solutions and notes that EHR vendors have little incentive to change things.

The Federation of State Medical Boards approves telemedicine guidelines that include a policy to apply the same standards of care for remote medical encounters as for in-person encounters. The guidelines also call for physicians to be licensed where the patient is located; for providers to establish a credible patient-physician relationship; and for an adherence to safety and privacy principles.
Meanwhile, an Idaho medical licensing board has fined a physician $10,000 for prescribing a patient an antibiotic while working for Consult-a-Doctor, a telehealth provider that has since been purchased by Teladoc. The Idaho Board of Medicine sanctioned the physician, who was licensed in the state, for prescribing medicine without an in-person examination of the patient. A group of telehealth-friendly legislators are now pushing stakeholders to establish standards for the practice of telemedicine.
Pay-for-performance programs unfairly penalize providers treating large numbers of poor people, according to a panel commissioned by the Obama administration. The panel notes that it is often harder to achieve successful outcomes when treating people who don’t have much income or education because low-income people may be unable to afford medications or transportation to doctors’ offices and the less educated may struggle to understand written instructions for home care and medication use. As a result, the existing payment policies unintentionally worsen disparities between rich and poor by shifting money away from doctors and hospitals that care for disadvantaged patients.
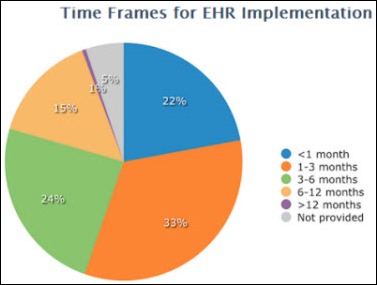
Forty percent of physician practices are looking to replace their existing EHR, according to a Software Advice report. Among buyers replacing their EHR product, the most common replacement reasons: the current solution is too cumbersome and/or integration is needed between applications. Mobile support for tablets and smartphones, e-prescribing, and lab integration were the most desired features among potential buyers. Based on the above time frames, it looks like a pretty good time to be selling EHR if you’ve got a good product.

MGMA Health Care Consulting Group’s Rosemarie Nelson offers insights into the use of kiosks in practices to improve RCM and patient satisfaction and cites several examples of practices that have reduced their claim denial rates and A/R days while also streamlining the patient check-in and registration process.
Email Inga.