News 12/11/23
Top News
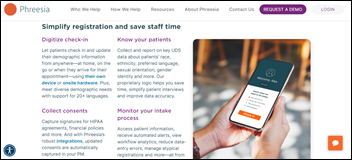
Patient intake software vendor Phreesia beats analyst expectations for Q3 2024 with a 25% bump in revenue to $91.6 million.
The company has within the last four months acquired medical answering service ConnectOnCall (for $14 million) and e-forms management and automation company Access.
Webinars
None scheduled soon. Previous webinars are on our YouTube channel. Contact Lorre to present or promote your own.
People

Angela Cosby (BayCare Medical Group) joins Walmart as VP of operations, healthcare delivery.
Announcements and Implementations
![]()
Kidney & Primary Care of Texas selects practice and care management services and software from Renal Care 360.
![]()
Complete Health will implement Relatient’s automated patient scheduling technology across its 24 locations across the Southeast.
Women’s Health Associates in Idaho will roll out Sunoh.ai’s ambient listening technology for clinical documentation.
Government and Politics

Lafourche Medical Group (LA) will pay HHS OCR $480,000 to settle potential HIPAA violations related to a 2021 phishing attack that exposed the PHI of 35,000 people. An OCR investigation found that the medical group had failed to conduct a risk analysis as required by HIPAA prior to the breach, and that it had no cybersecurity review policies in place.
Sponsor Updates
- AdvancedMD earns its Electronic Prescribing for Controlled Substances recertification from the Drummond Group.
- Medicomp Systems releases a new “Tell Me Where It Hurts” podcast featuring Bob Taylor, DO, chief product strategies of TouchWorks EHR, Altera Digital Health.
Blog Posts
- Nurses of Note 2023: The Lead Director for Ambulatory Care Management (PerfectServe)
- Smart Coverage Detection Equals Better Patient Care + Stronger Bottom Line (EClinicalWorks)
Contacts
More news: HIStalk.
Get HIStalk Practice updates.
Contact us online.
Become a sponsor.

















Re: Walmart Health: Just had a great dental visit this morning, which was preceded by helpful reminders from Epic, and…