News 4/13/26
Top News
Vibrant Practice rebrands to Ultralight and announces $9.3 million in new funding. The company offers EHR software to longevity and personalized medicine clinics.
Sponsored Events and Resources
None scheduled soon. Contact Lorre to have your resource listed.
Acquisitions, Funding, Business, and Stock
HeyDonto AI Technology raises $20 million in seed funding. The company’s Conduit platform connects dental practice management systems with medical EHRs, consumer health apps, and payer systems.
People

Lalan Wilfong, MD (Thyme Care) joins Navista as chief medical officer.
Announcements and Implementations
Mental Wealth Solutions announces GA of HealthcareCheck, a white-label patient screening and social care coordination app for FQHCs, behavioral health clinics, and dialysis clinics.
Athenahealth adds Rater8’s provider reputation management capabilities to its AthenaOne platform.
CareAxis launches to offer automated patient engagement software to multi-provider practices.
Other
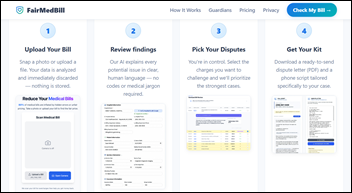
The local news profiles FairMedBill, a startup that uses patent-pending, AI-based software to review medical bills for possible errors and offer guidance on how to dispute them. Husband-and-wife team Kelly and Kasha Williamson launched the company after experiencing their own frustrations with medical bills: “From our perspective,” says Kasha, “we’re not looking to Silicon Valley, we’re not looking to cash out. This is really out of a feeling of wanting to be able to help people who are in a bad situation.”
Patients express frustration with ongoing Palomar Health Medical Group (CA) technical difficulties that have impacted their ability to schedule appointments and communicate with clinicians. The group sent a letter to patients March 13 explaining that it was working with NextGen, its EHR and practice management systems vendor, to resolve the issues. No further updates have been provided and patient portal messaging is still down.
Contacts
More news: HIStalk.
Follow on X, Bluesky, and LinkedIn.
Get HIStalk Practice updates.
Contact us online.
Become a sponsor.





















The article about Pediatric Associates in CA has a nugget with a potentially outsized impact: the implication that VFC vaccines…