News 3/23/26
Top News

Doctronic announces $40 million in Series B funding, bringing its total raised to $65 million. The company offers an AI healthcare chatbot that can, for an additional fee, connect users to virtual providers.
Sponsored Events and Resources
None scheduled soon. Contact Lorre to have your resource listed.
Acquisitions, Funding, Business, and Stock
Senior-focused primary care optimization company Oasis Health Partners acquires RCM and practice management business Premier Health.
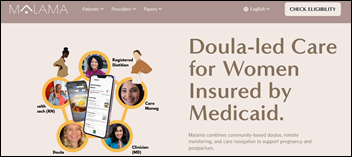
Hybrid maternal care provider Flourish Care raises $5.7 million in seed funding. The company, which offers its doula-centered services in 18 states, will use the funding to improve its data platform and expand nationally.
People

Archie Mayani (GHX) joins Evolent Health as chief product officer.

Office Practicum promotes Jennifer Reale to CFO.



Experity names Jason McNeil (ModMed) EVP of RCM, Clarissa Riggins (Experian) chief product officer, and Nick Maynard SVP of sales.
Announcements and Implementations
PointClickCare announces GA of its EHR for practice groups.

Your Health implements Fathom’s autonomous coding platform across its 14 offices in Georgia and South Carolina.
Other

Well Health Technologies intends to throw its hat in the ring when the Ontario government begins considering vendors for a province-wide EHR as part of its Primary Care Action Plan Program. Nearly 1,700 clinics in the province already use EHR software from its Wellstar subsidiary.
Contacts
More news: HIStalk.
Follow on X, Bluesky, and LinkedIn.
Get HIStalk Practice updates.
Contact us online.
Become a sponsor.


















The article about Pediatric Associates in CA has a nugget with a potentially outsized impact: the implication that VFC vaccines…