The article about Pediatric Associates in CA has a nugget with a potentially outsized impact: the implication that VFC vaccines…
News 8/28/12
From Sleepless “Re: Practice Wise. Julie McGovern’s ‘One Project at a Time’ article was great! If only the business world really would acknowledge how much disruption it creates and the resulting levels of frustration.” Sleepless is referring to Julie’s recent post, which addresses the hard work of EHR implementations and how clinics would be prudent to avoid tackling multiple large initiatives simultaneously. She offers some great tips, beginning with:
If other initiatives must be tackled, try to stage the projects to preserve the sanity of everyone involved.
The one-year delay for the ICD-10 code set is confirmed by HHS Secretary Kathleen Sebelius and the new compliance date is October 1, 2014. Following the announcement, MGMA expressed concerns that HHS didn’t undertake due diligence to ensure ICD-10 won’t disrupt cash flows and recommended additional ICD-10 pilot testing before a full roll-out. Meanwhile, the AMA issued a statement recommending “CMS delay the move to ICD-10 by a minimum of two years.”
RCM provider ZirMed hires Kenneth Willman (Humana) as VP of payer solutions and strategy.
I read this profile on startup HealthTap and am not convinced of the model’s viability. HealthTap allows patients to pay $10 to have a secure, private conversation with a physician in a format similar to email. Patients can share documents and images and the doctor then analyzes the case. The patients can choose a physician to engage with “out of a million” in HealthTap’s database (or 14,000 licensed US doctors.) I understand how this could be attractive to a patient, though I have to wonder what kind of doctor would be willing to participate. The company says their site allows physicians to use their knowledge to “build an image” and as a business development tool. I thought we were facing a doctor shortage, not a patient shortage, so how many physicians – particularly quality primary care doctors – really need to recruit more patients? What am I missing?
Emdeon expands its Clinical Exchange solution to include e-prescription routing, lab orders and results exchange, care alerts, medication history, and clinical messaging.
More evidence of telemedicine’s growing popularity: in a survey of 440 mid to large size firms, 9% indicated they had plans to offer telemedicine consultations in 2013; another 27% are considering them for 2014 or 2015.
simplifyMD adds billing software provider Healthpac as a reseller for simplyMD’s EHR.
Seventy-five percent of 21,000 physicians participating in a Medscape survey say they use an EHR system, while an additional 20% plan to adopt one in two years. That sounds high to me, but adoption is no doubt trending up. The top-ranked EHRs among smaller practices were Amazing Charts, VA-CPRS, and Practice Fusion, while groups with 25 physicians or more favored VA-CPRS, Epic, e-MDs, and Medent. The most widely used EHRs were Epic, Allscripts, and Cerner.
Last week on HIStalk we mentioned some key items from the Stage 2 MU final rule, which was published last week. A few items impacting EPs include:
- Stage 2 will begin in 2014, a full year later than the date published in the original ARRA legislation. Providers have two years after achieving Stage 1 to achieve Stage 2.
- Providers don’t have to achieve Stage 1 MU until 2017, though Medicare penalties will begin in 2015.
- EPs have a new core measurement requiring at least 5% of patients seen by the EP to use secure messaging to communicate health information.
- Hospital-based physicians who can demonstrate they funded the purchase, implementation, and maintenance of an EHR without reimbursement from the hospital and use the EHR in place of the hospital’s EHR can apply to receive a MU payment.
- Certain physicians that don’t have a lot of face-to-face time with patients can apply for an exemption to the MU program to avoid Medicare penalties. Exceptions are also possible for physicians that live in geographic areas without sufficient Internet access and those subject to unforeseen circumstances, such as natural disasters.




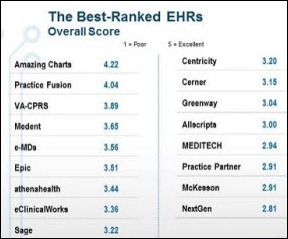







So, the top rated EHRs are either free or nearly-free? How is it that the VA system gets such high marks?
For Healthtap… I agree very few PCPs will have time for this – but I believe the physician attraction is more about specialists getting referrals. So if you have some weird stomach pain, a GI doctor will tell you “it might be this or that… you should get a colonoscopy”… and then hope that they want to see him. So optimistically, it’s a way to get patients to realize they might need to appropriately see a specialist or get a procedure. The pessimist might say it’s a way for specialists to churn the waters and get more people doing more stuff so they can make more money. I wonder if the tides will turn when the specialists have a capitated contract with ACOs and get paid a set salary no matter how many colonoscopies they do?
Gentleman (or ladies)… strap on your research hats! Would be an interesting experiment for someone to ask a set of questions today… then wait 5 years and ask them again. Assuming the reimbursement system has changed, wonder if the answers will be different. For example, today they might say “Get a Colonoscopy”, but in five years- would they say “Cut out dairy for a month, and if that does not work, then cut out wheat for a month, and if that does not work, then see someone”. Hope someone has the patience and foresight to do this