The article about Pediatric Associates in CA has a nugget with a potentially outsized impact: the implication that VFC vaccines…
DOCtalk with Dr. Gregg 12/17/15
E-Prescribing in the Dark
I don’t know about anybody else’s experiences, but my relationship with e-prescribing reminds me of Helen Keller’s quote about “walking with a friend in the dark.”
Not having seen much posted about this topic may be more a result of my ignorance than anything, but a quick search didn’t lead to many practical perspectives that I could find. Thus, maybe adding one to the blogosphere wouldn’t be just a rehash.
First, we’ve used e-prescribing for years. Love it. Period. When it works.
And it mostly does work, and typically works quite well. It makes it easy to prescribe, reduces the risk of error from illegible handwriting, lowers the chances of lost prescriptions to almost null, and makes tracking of prescribed meds MUCH easier.
But, all of that’s true only when it works. As mentioned, it doesn’t always work, and that’s when the dark creeps in.
(The e-prescribing solution that our EHR employs has been called the “giant” of the industry. There are others, and they may work differently, but my experience is limited to our little giant.)
The two main times I’ve noted when it doesn’t work:
- When something is amiss in the patient demographics
- When an “Unknown Drug” gets pulled into the patient record
The first issue is really problematic. If our system sends an inquiry to the e-prescribing solution and there’s some kind of glitch in the demographics, here’s one of the responses we receive:
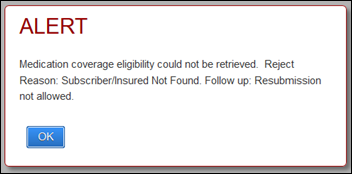
I ask you: What do you do with that? There are no instructions, no next steps. You’re only told that this person, who you know for a fact exists and whose insurance eligibility you’ve verified, can’t be found. And you’re not allowed to do anything about it. (“Resubmission not allowed.”)
There are some similar rejection notices as I recall, but they all have the same thing in common – no info on what exactly is wrong, no way to correct whatever errors there are, and no option to do anything about it.
The second problem isn’t always quite as vexing, but still should have some improved address. Here’s an example from one of my patient’s charts (patient and prescribing doctor de-identified):
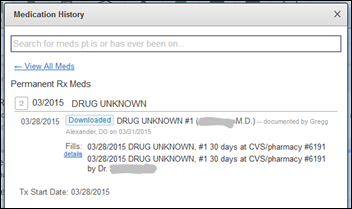
With this one, I can at least call the pharmacy and try to determine which of the medications this patient was dispensed on that day might be the elusive “DRUG UNKNOWN.” This involves figuring out which CVS pharmacy is “#1691,” finding their phone number, calling them to ask them to look up prescribed Rx from that day for that patient, and then manually charting the now known drug into the patient’s chart. As I said, problematic, but at least it has a resolution, even if it isn’t simple or one automated by the e-prescribing solution.
My personal ask for our (or any) e-prescribing solution is this: You’re good to have as a friend. I appreciate you. Walking with you even though it’s sometimes in the dark is far better than walking without you. But, please … please … add transparency and end user-friendly info and advice. Cryptic messages that provide no value or direction may make some programmer on your end feel as though they’re doing something, but it isn’t something that’s at all helpful to us provider grunts – be they us little trench grunts or those in the bigger trenches. We would all benefit from a little more light.
From the trenches…
“Walking with a friend in the dark is better than walking alone in the light.” – Helen Keller

Dr. Gregg Alexander, a grunt in the trenches pediatrician at Madison Pediatrics, is Chief Medical Officer for Health Nuts Media, an HIT and marketing consultant, and sits on the board of directors of the Ohio Health Information Partnership.
Contacts
Jennifer, Mr. H, Lorre, Dr. Jayne, Dr. Gregg, Lt. Dan
More news: HIStalk, HIStalk Connect.
Get HIStalk Practice updates.
Contact us online.
Become a sponsor.








Thanks Dr Gregg for posting this. Our organization through its members developed the SCRIPT standard, which is used by vendors to implement ePrescribing. Unfortunately there are over 600 vendors and each although certifying that their application can send a prescription, often each leaves their user such as you questioning why issues like this come up. Our organization has developed a task group to look into “best practices” for eprescribing, and with this task group have uncovered user issues such as what you are seeing. I would strongly recommend your comments are seen and understood by your vendor. That is truly how problems like this get fixed. As you have said and most physicians have attested, eprescribing is the next best thing to sliced bread when it works! Thank you again.
John Klimek R.Ph.
SVP Standards and IT
NCPDP