News 1/20/25
Top Posts
Knack RCM, which provides revenue cycle services to ambulatory providers and durable and home medical equipment suppliers, acquires HealthyBOS, a DME-focused revenue cycle company based in the US and the Philippines.
Webinars
January 23 (Thursday) 11 ET. “Maximizing Revenue With Minimal Resources: Work Smarter, Not Harder in Claims Management.” Sponsor: Inovalon. Presenter: Travis Fawver, senior sales engineer, Inovalon. Navigating the challenge of hitting revenue goals is daunting, but billing doesn’t have to be. The presenter will explore how strategic adoption of new technology can transform claims management processes from reactive to proactive. Learn how to reduce denials while empowering staff to focus on high-value activities, and gain proven strategies to simplify workflows, automate routine tasks, and build a more efficient RCM operation to maximize reimbursement.
Stream on demand. “Healthcare Data Security: Aligning Processes with Evolving Threats & Regulations.” Sponsor: Inovalon. Presenters: Anthony Houston, MBA, senior director of security, risk, and compliance, Inovalon; Paul Wilder, MBA, executive director, CommonWell Health Alliance; Luke McNamara, MPA, deputy chief analyst, Google Cloud; Michael Quinn, VP of strategic partner development, Inovalon. Hear leaders in healthcare data security discuss some of the top recent threat evolutions and how organizations can proactively respond by making ongoing improvements to security protocols.
Previous webinars are on our YouTube channel. Contact Lorre to present or promote your own.
Announcements and Implementations
NextGen Healthcare adds gastroenterology-specific workflows to its EHR software.
Ascend Medical, which offers in-office, virtual, and home-based care in Georgia and Texas, creates a patient app using digital front-door technology from Amenities Health.
The Sequoia Project designates EClinicalWorks a QHIN.

Capital Digestive Care implements Latica’s data insights platform for improved visibility into internal metrics, development of new care pathways, and the ability to access and contribute to gastrointestinal research via Latica’s GI data repository.
Contacts
More news: HIStalk.
Follow on X, Bluesky, and LinkedIn.
Get HIStalk Practice updates.
Contact us online.
Become a sponsor.




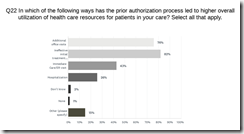






















The article about Pediatric Associates in CA has a nugget with a potentially outsized impact: the implication that VFC vaccines…